Service description for patients
1. description of the concept
1.1. Principles
People with chronic illnesses can have high and complex needs for outpatient care, medication and nutrition. A critical aspect of outpatient treatment is the coordination of the necessary care and the coordination of the partners involved. The Outpatient Partner addresses these needs and embodies digitally supported care management. The AP concept (hereinafter “AP concept”) includes a combination of coordinative services with the digital management platform “APST care portal” (hereinafter “APVP”). Ambulanzpartner Soziotechnologie APST GmbH (hereinafter referred to as “APST”) offers care management services that serve to improve coordination, communication and networking between patients (and their relatives), doctors and medical assistants in practices, outpatient clinics and hospitals (“medical partners”) as well as providers of drug therapy (pharmacies, manufacturers of drugs and medical devices), nutritional therapy and providers of remedies and aids (“care partners”). The APVP Internet platform is the communication and management platform on which care coordination is digitally supported, linking an electronic care record with digital process control for the purpose of care management and care research. Coordinators implement care management for necessary medications, medical devices, aids and remedies as well as specialized care in personal, telephone or electronic contact with patients (and their relatives), medical partners (doctors, social services) and care providers. The care management offered by APST includes services that are not provided within standard care or are provided to a lesser extent. The standard care provided by doctors and other service providers remains unaffected by the AP concept. The determination of the need for care, including the medical indication for medication and other medical products as well as aids and remedies, is the unrestricted responsibility of the doctor. The assessment of the appropriateness and cost-effectiveness of care also remains the unchanged responsibility of the doctor and payer. The services and use of the APVP only come into effect once the care decisions have been finalized by the doctor in a doctor-patient contact. The offer to participate in the AP concept is based on the patient’s wish and voluntary cooperation. The patient has full participation rights at all times and is only supported to the extent desired. The patient is entitled, informed and able to terminate participation in APST care management at any time and without giving reasons.\
The AP concept is offered to patients under the following special conditions.\
a) For diseases with special conditions:
- Serious illness
- Complex chronic disease
- Rare disease
b) For a supply with special conditions:
- High organizational expenses in care for patients and medical partners
- High need for specialization to ensure the quality of care
- High need for coordination between various medical partners and providers
- High demand for healthcare research
The AP concept is offered for use in particular for patients with the following diagnoses and syndromes due to special medical conditions and care requirements:
- Amyotrophic lateral sclerosis (ALS)
- Spinal muscular atrophy (SMA)
- Spastic spinal paralysis (SSP)
- Parkinson’s syndrome (severe or special course)
- Multiple sclerosis (severe or special course)
- Defect syndrome after stroke (severe or special course)
- Defect syndrome after traumatic brain injury (severe or special course)
- Dementia syndrome (severe or special course)
- Tetraparesis
- Hemiparesis
- Spasticity syndrome
- Cachexia syndrome
- Dysphagia syndrome
1.2. Supply management
In the standard care of patients with chronic, serious or rare diseases, the doctor determines the need for aids and remedies, medication, nutritional therapy or other medical products as part of the treatment. The determination and discussion of the need for treatment takes place independently of the APST concept and the patient’s possible participation in APST care management. The doctor informs the patient about the option of participating in the AP concept if the patient can benefit from digitally supported care coordination. It is made clear that the doctor will not receive any remuneration or other benefits for this recommendation. Another reason for non-binding information about the possibility of participating in the AP concept is if the patient meets the criteria for participation in a care research study (see 1.3.). The designation by the doctor is one of several ways in which the patient can be informed about the AP concept. Other information channels include recommendations from self-help organizations and patient associations, testimonials in blogs and other social media, the APST website and publications about the AP concept in print and online media and scientific publications. If and insofar as requested by the patient, the APST provides services on behalf of patients that would otherwise have to be provided by the patient or relatives themselves but cannot be provided or cannot be provided adequately due to a lack of resources and skills (e.g. searching for suitable care providers; arranging appointments; providing documents, statements, etc.). In addition to care coordination, digital networking across professional groups (via the APVP internet portal) is a further service that has not yet been included in standard care; if the patient wishes to participate in the AP concept, the necessary documents are made available to the APST. On the basis of informed consent, the patient commissions APST to provide the entire care management or individual services. To this end, the patient or a legal representative signs a declaration of consent authorizing care management by APST and the digitalization of personal data on the APVP internet platform. Once the necessary declarations have been submitted, an electronic care file is created and the patient is contacted by a care coordinator from APST or a medical partner. The care process is described in detail in section 2. The order is placed with the care provider regardless of whether the selected care partner makes use of the APST services.
1.3. Health services research
The AP concept pursues a dual approach: data generated in the context of care management is used for a systematic analysis of care based on the informed consent of patients. This creates a “double effect”: the digitization of care data on the APVP directly serves the coordination of care and, at the same time, care research through the evaluation of “routine data” (data from standard care). All patients who make use of APST care management are also invited to take part in a registered study in which medical data on medication and nutritional care, the provision of aids and remedies and socio-medical data are scientifically evaluated and published for the purpose of care research. Consent for health services research in the AP concept is given on the basis of separate study information and a separate declaration of consent.
1.4. Principle of the open network
Voluntariness, optional use and the unconditional option to end participation are the basic principles of the AP concept. It is therefore possible to coordinate care within the AP concept, while other care is provided outside the AP concept, either in parallel or at a different time. Care partners can make use of the APST services or terminate their participation without any formal barriers. The entirety of participating patients, care partners, medical partners and coordinators is referred to as the care network. The participation of patients, care partners and medical partners in the AP concept is dynamic and has the character of an open platform.
2. supply management
2.1. Provision of medical aids 2.1.1 Addressed needs for the provision of medical aids
For people with chronic neurological conditions, the focus is on aids for mobility, transfer and communication. Identifying a suitable care partner is particularly relevant for rare, severe and progressive diseases. In the case of rare and severe diseases, individual care concepts are necessary in the segments of orthotics, mobility, transfer and communication aids, which require a high level of professional and technical expertise from the care provider. In the case of progressive illnesses, it is advantageous for care providers to have detailed knowledge of the underlying clinical picture in order to anticipate the course of the illness and the expected increase in deficits and to incorporate this into the concept for the provision of assistive devices. The principle of anticipatory provision of assistive devices serves to avoid incorrect provision and requires the provider to have experience in the specific indication. Overall, from the patient’s perspective, there is a justified interest in receiving care from service providers who (in addition to their formal qualifications) have specific expertise in the underlying disease and assistive technology constellation to be treated. Identifying and contacting experts in the provision of assistive technology devices is advantageous in order to maximize experience, quality and efficiency in the treatment of assistive technology devices and to reduce the risk of incorrect treatment. The APST’s services initiate networking with specialized providers on behalf of the patient and support them in the further course of care.
2.1.2. Procedure for the provision of aids
The provision of medical aids is a complex process that involves considerable time, organizational and administrative effort. Fig. 1 shows the necessary chain of action between patient, provider and doctor to ensure that a suitable assistive device is submitted to the health insurance company for reimbursement. The structure of the process is not changed by APST’s care management and follows the formal requirements of healthcare provision. However, the APST’s service consists of taking over, coordinating and digitizing certain organizational steps in the communication between patient, provider and doctor on behalf of the patient and the provider. The coordinative service and the use of the APVP internet platform relieve the burden on patients and care partners.
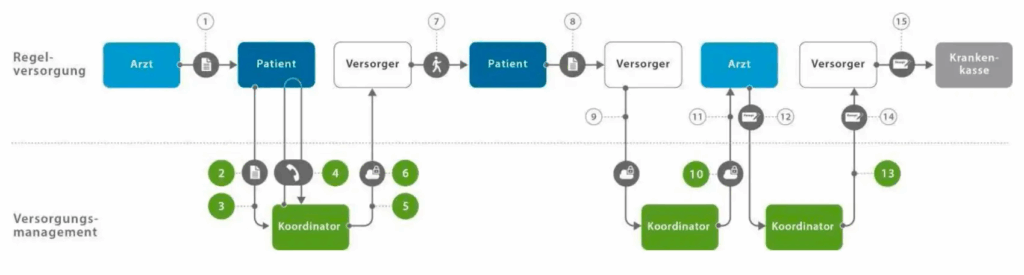
Fig. 1: Procedure for the provision of aids: The provision of assistive devices follows a structured process that is realized in the following sub-steps. 1) the doctor makes an indication for an assistive device; 2) the patient commissions the coordinator to assist with the provision of assistive devices (request for provision); 3) the coordinator receives the request for provision; 4) the patient confirms the request for provision; 5) the coordinator identifies a suitable provider of assistive devices; 6) the provider receives and confirms the request for provision; 7) the provider visits the patient and draws up a proposal for provision; 8) the patient confirms the care proposal; 9) the provider sends the prescription proposal; 10) the coordinator sends the prescription request to the doctor; 11) the doctor checks the prescription request; 12) the doctor prepares and sends the prescription for the assistive technology device; 13) the coordinator receives and sends the prescription to the provider; 14) the provider receives the prescription; 15) the provider applies for the costs to be covered.
2.2. Provision of remedies
2.2.1. Addressed requirements for the provision of remedies
There is a high demand for specialized physiotherapy, occupational therapy and speech therapy for severe or rare diseases. Therapy practices that have special skills or care options for certain illnesses are of interest. Specialized therapy practices with qualifications and experience in treating the indications listed in 1.1. are of particular relevance. Special care conditions can also arise in the case of common illnesses (e.g. stroke) (physiotherapy after botulinum toxin treatment of spasticity; combination of therapeutic care with the provision of assistive devices). A frequent search criterion is therapy practices that can provide high-frequency therapy (4-5 times per week) in home visits. Patients with specific needs for the provision of therapeutic appliances (special form of therapy; high-frequency therapy, home therapy, specific interdisciplinary experience with accompanying pharmacotherapy, orthoses or palliative aids, etc.) ask the APST to find a suitable care partner. In the further course of treatment, the focus is on organizational support with the provision and sending of necessary reports and other documents as well as the coordination of therapy with other treatment providers (e.g. occupational therapy and speech therapy), aid providers (e.g. orthopaedic mechanical workshops) or care providers (coordination of nursing or therapeutic measures). In the case of severe and chronic illnesses, medical aid providers play a central role in the care concept. Particularly in the case of high-frequency therapeutic care (several times a week), the therapeutic care provider is the professional group that implements the medically indicated care concept in direct contact and with maximum intensity. Due to the direct interaction between patient and provider, detailed specialist knowledge, experience and psychosocial skills that go beyond formal qualifications are required, particularly in the case of progressive illnesses and palliative treatment goals. Against this background, there is a legitimate interest from the patient’s perspective in receiving care from a healthcare provider who has the therapeutic expertise, the necessary experience and the required psychosocial competence.
2.2.2. Procedure for the provision of remedies
The APST care management system helps patients to find and contact specialized physiotherapists, occupational therapists and speech therapists. In the case of long-term or permanent therapy, it is necessary to provide the necessary prescriptions, which in standard care are communicated by the therapist to the patient, who in turn communicates the need for the prescription to the prescribing doctor. Once the indication has been checked, the patient receives the follow-up prescription and submits this document to the provider. This administrative process (especially for patients with mobility and communication barriers and in the case of parallel use of different remedies) is associated with high costs for the patient. Coordinators of theAPST relieve this organizational process — on behalf of the patient – through document management and the use of the APVP Internet platform. The upper part of Fig. 2 shows the necessary organizational steps in standard care. The lower part of the schematic diagram shows those sections of the care process in which patients and healthcare providers receive coordinative support.
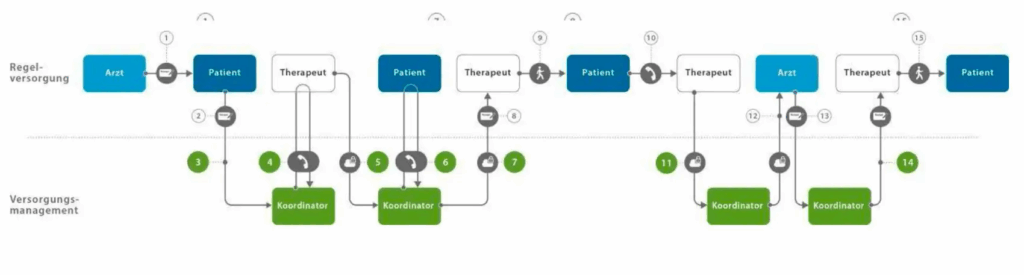

Fig. 2: Procedure for the provision of therapeutic products: The provision of remedies follows a structured process, which is realized in the following sub-steps. 1) the doctor provides the indication for the provision of remedies and issues the prescription; 2) the patient instructs the coordinator to assist with the provision of remedies (request for provision) and sends the prescription to the coordinator; 3) the coordinator receives the prescription for remedies; 4) the coordinator identifies a suitable therapist and submits a care request; 5) the therapist accepts the care request; 6) the coordinator proposes a therapist to the patient; the patient confirms the proposed therapist; 7) the therapist receives the care order; 8) the therapist receives the prescription; 9) the therapist treats the patient; 10) the patient requires further treatment after completion of the therapy and a prescription required for this; he instructs the therapist to formulate a prescription proposal; 11) the therapist sends a prescription proposal for further treatment; 12) the coordinator submits the prescription request to the doctor; 13) the doctor checks the prescription proposal, determines the indication for continued (or modified) treatment, prepares and sends the prescription; 14) the coordinator receives and sends the prescription; 15) the therapist takes over the patient’s further treatment.
2.3. Medication supply 2.3.1 Addressed needs of the medication supply
In the case of complex and rare diseases, there may be special requirements for the supply of medicines that relate to the following areas of pharmacists’ responsibilities:
- Advice on medicines
- Production of recipes
- Cooperation with care partners from other healthcare professions
2.3.1.1. Advice on medicines Providing advice on the effects and side effects and supporting the proper use of medicines is one of the pharmacist’s regular tasks. In the case of complex and rare diseases, however, it is advantageous if the pharmacist has special expertise in these diseases. In this way, empirical knowledge of dose-effect relationships and side effects can be incorporated into the pharmacist’s advice on the effects and risks of medicines and their appropriate use. There is a need for specialized advice in the event of an increased risk of adverse drug reactions and in the case of drug therapy in an area of application outside the indication or a changed type of application (off-label use). The AP concept coordinates the care of patients who have a special need for advice, in particular due to the following conditions of use:
- Dysphagia (swallowing disorder)
- Sialorrhea (uncontrolled salivation)
- Percutaneous endoscopic gastrostomy (artificial feeding by tube)
In the case of complex and rare diseases, there may be special consultation circumstances and thus special communicative and psychosocial requirements for the pharmacist and other pharmacy staff as well as for the technical infrastructure of the pharmacy. The AP concept coordinates the care of patients who have a particular need for advice due to the following circumstances:
- Restriction or loss of the patient’s speech production during the consultation
- Loss of telephony and necessary use of digital media in the consultation and further communication process
- Locked-in syndrome (loss of mobility and communication with preserved intellectual functions)
2.3.1.2. Production of recipes The preparation of formulations is one of the pharmacist’s regular tasks. There is a specialized need when rare formulations have to be developed, produced and stocked. In particular, the AP concept coordinates the care of patients who have a special need for the preparation and timely supply of prescriptions for the following groups of medicines:
- Anticholinergics for the treatment of sialorrhea
- Cannabis-containing medication for the treatment of cramps, spasticity and fasciculations
- Spasmolytics containing 4-aminopyridine for the treatment of spasticity
- Dextromethorphan-containing medication for the treatment of motor disinhibition
2.3.1.3. Cooperation with care partners from other healthcare professions
Cooperation with other healthcare professionals is part of the pharmacist’s regular duties. In the case of complex, rare and chronic diseases, there is a particular need for cooperation in order to ensure advice on drug risks and the appropriate use of medication. The AP concept coordinates the care of patients who require special coordination between the pharmacist and care partners:
- Provider of PEG tubes: The administration of medication via a PEG tube is an interdisciplinary task and requires special expertise from all those involved, as medical, nursing and pharmaceutical aspects must be taken into account. Ideally, data should be recorded for each individual patient, the suitability of the medication for PEG should be assessed by the pharmacist and the final check and prescription should be carried out by the doctor. Targeted advice for nursing and nutritional care providers by the pharmacist ensures the proper handling of PEG tubes and drug safety. Damage to feeding tubes caused by medication can be prevented.
- Healthcare providers: Information about salivary flow-modified drugs is important for the success of speech therapy treatment. At the same time, information from speech therapists about sialorrhea is included in the pharmacist’s advice on the appropriate use of oral medications. For physiotherapists and occupational therapists, knowledge of sedative, psychotropic or spasmolytic medication is relevant for therapy planning and ensuring the success of therapeutic treatment. Conversely, information from physiotherapists and occupational therapists can be important for advising pharmacists on effects (e.g. improvement of gait disturbances due to spasmolytic medication) and risks (e.g. risk of falling due to spasmolytic medication).
- Assistive technology providers: For providers of mobility, transfer and communication aids, knowledge of over-sedating, psychotropic or spasmolytic medication is relevant for the testing and suitability of assistive technology and the avoidance of incorrect care.
2.3.2. Procedure for supplying medication The APST care management system supports patients in finding and contacting specialized pharmacists. In the case of long-term or permanent medication treatment, patients are relieved of organizational tasks by APST coordinators and by using the APVP internet platform.Fig. 1 shows the organizational process of medication supply and those stages in the supply process where patients or pharmacists receive coordinative support.
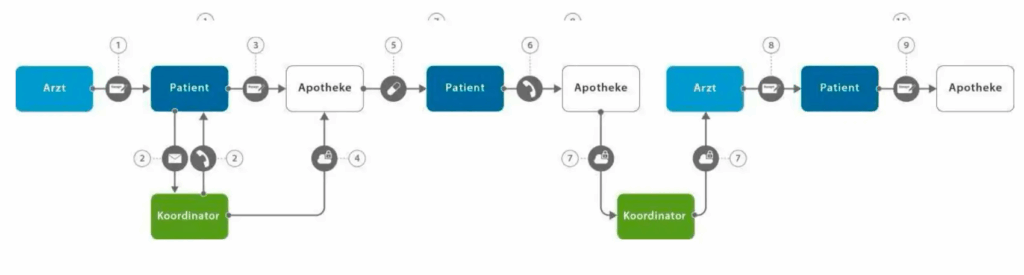
Fig. 3 Medication supply process: The supply of medication follows a structured process, which is realized in the following sub-steps. 1) the doctor provides the indication for the medication, writes the prescription and hands the prescription to the patient; 2) the patient instructs the coordinator to search for a suitable pharmacist (supply request); the coordinator identifies a suitable pharmacist and informs the patient of this; 3) the patient sends the prescription to the pharmacist; 4) the pharmacist receives the supply-relevant data via the outpatient partner supply portal; 5) the pharmacist contacts, advises and supplies the patient; 6) for the follow-up medication, the patient asks the pharmacist for a suggestion regarding the medication requirement; 7) the pharmacist sends his suggestion regarding the medication requirement to the doctor via the outpatient partner care portal; 8) the doctor provides the indication for the continued (or changed) medication supply and sends the prescription to the patient; 9) the patient sends the prescription to the pharmacist (continuation of the process)
2.4. Guaranteeing freedom of choice
The patient’s participation in APST care management requires the patient’s informed and documented consent. This requires the acknowledgement, consent or selection of options and signing of the following documents:
- General Terms and Conditions for Patients (GTC)
- Privacy policy for care management and care research by Ambulanzpartner Soziotechnologie APST GmbH and the use of the Ambulanzpartner care portal
- Declaration of consent for participation in care management and care research by Ambulanzpartner Soziotechnologie APST GmbH and for use of the Ambulanzpartner care portal
- Declaration on the free choice of pharmacy (if medication supply is desired)
- Delivery order for pharmacies (if applicable)
- Release from confidentiality obligations for pharmacies (if applicable)
When participating in care management, the patient has comprehensive freedom of choice: they can fill their prescription themselves or choose a specific provider to be commissioned by the care coordinator or instruct the APST coordinator to identify a suitable provider and coordinate the care. In the document “Declaration on free choice of pharmacy”, the patient confirms that they have been informed about the right to choose a pharmacist and about these options and that they have decided in favor of one of these options by signing it. Within the framework of care coordination, it is possible under the legal requirements to deliver medication by courier or by mail order to the patient’s home of origin or to a doctor’s practice where the medication is administered (e.g. injection or infusion therapy). For this purpose, the patient signs the “delivery order” document authorizing a pharmacy or a logistics company commissioned by the pharmacy to deliver the medication by courier or mail order.
3. description of the services
The services are used for communication and networking between patients, doctors and care partners and can be used together or as individual components. The modular AP service architecture consists of the following components:
3.1. Supply coordination
Care coordination is a service provided by non-medical coordinators at APST. It includes organizational tasks in the provision of aids and remedies as well as medication and medical devices. Care coordination includes the following services:
- Receiving supply requests by e-mail and fax as well as by post or online
- Digital recording of the supply request
- Telephone contact with the patient, relative or legal representative to confirm and specify the care request
- Identification of a suitable provider on behalf of the patient
- Care request to a suitable provider on behalf of the patient
- Provision of a telephone service for patients, medical partners and care partners
- Control and reminder service for unprocessed supply requests to supply partners
3.2. Data management
Data management is a service provided by coordinators and data managers. It includes the collection of medical information and care data as well as its digitization and provision to patients, care partners and medical partners. Data management includes the following services:
- Telephone contact with patients, relatives or legal representatives to collect master data, medical data and care data
- Digitization of master data, medical data and care data in the electronic care file of the APVP Readout of doctor’s letters and other medical documents to record and digitize diagnostic data according to ICD-10
- Reading doctor’s letters and other medical documents to record and digitize care data
3.3. Document management
Document management is a service provided by coordinators and data managers. It includes the receipt, recording, archiving and provision of medical documents. Document management includes the following services:
- Collection and mailing of printed documents (e.g. doctor’s letters, therapy reports, medication plans, care requests, trial protocols)
- Scanning, indexing, uploading and versioning of documents (e.g. doctor’s letters, therapy reports, medication plans, care requests, trial protocols)
- Creation, circulation and versioning of document templates (e.g. medication plans, care requests, forms)
3.4. Complaints management
Complaint management is a service provided by coordinators on behalf of patients and care partners. Complaints from patients and medical partners are received, systematically recorded, clarified, evaluated and communicated to the partners involved (patient, care partner and, if applicable, medical partner) via a telephone service as well as an e-mail and inbox. Complaints management includes the following services:
- Provision and evaluation of complaint forms as well as telephone complaint acceptance, provided that no medical-pharmaceutical issues are involved
- Reviewing and communicating criticized care processes to patients, doctors and providers, provided that no medical-pharmaceutical issues are involved.
3.5. Patient reviews
Patients or persons authorized by them also have the opportunity to evaluate medical devices and medical services. Through the cooperation of the patient, an important contribution to the improvement of healthcare can be made or targeted suggestions for improvement can be made to optimize future medical devices, treatments and care processes. Patient assessments are carried out by trained personnel. The assessment involves interviewing patients in direct contact, by telephone or by e-mail.
The patient assessment includes the following services:
- Creation of interview documents (print) and configuration of interview software (online, e-mail dispatch)
- Conducting telephone surveys, direct surveys, sending out online assessments
- Evaluation of patient assessments
- Presentation of patient assessments on the APVP and other communication channels (newsletter; print media, publications)
4. description of the Outpatient Partner Care Portal (APVP)
The APVP internet platform(https://www.ambulanzpartner.de) is the digital communication and management platform used to document and control all care management services. It is the communication medium between the professional coordinators and care partners in order to manage the provision of medical aids and remedies or the supply of medication and nutrition. Patients can make use of the care management services without using the APVP software or any other computer application themselves. As a result, patients can also participate in the AP concept without technical knowledge or access to the Internet. Patients and medical partners are given the option of obtaining their own access to the APVP Internet portal. This access gives patients and medical partners the option of viewing the organizational and communication processes between the coordinators and care partners. Patient and care-related data is recorded on the APVP, which is presented in 4.2. Specific access authorizations have been defined for access to personal data, which are described in 4.1.
4.1. User roles and authorizations
A central feature of data protection is the limitation of access rights to the data required for the user role. This means that not every user of the AP portal can view all the data stored there. The limitation of data access was specified for the following user groups.
4.1.2. Medical partners and supply partners
- All data in the portal of those patients for whom there is a treatment or care order (no data availability of patients for whom there is no order for action)
4.1.3. Coordinator role
- All data in the portal for those patients for whom a coordination order exists (no data availability for patients for whom no coordination order exists)
4.1.4. Network manager, data manager and administrator roles
- Complete data set of all patient and care-related data
- Complete data set of all medical partners and care partners
- Complete data from patient evaluations (survey management) and participant groups (participant management)
4.2. Data provided Extensive patient and care-related data is recorded and stored on the AP Internet portal on the basis of the patient’s detailed consent in a systematic menu navigation using free text or selection lists. The data fields are to be understood as input options that are not recorded for every patient and every care process
Data provided
| Data category | Data fields |
| Contact date | – Main address – Secondary addresses – Telephone numbers of the patient (lists) – Telephone numbers of relatives and other authorized persons (lists) – Type of living space (house, apartment; rented, owned) – Living space with a number of rooms – Number of steps if stairs are present – Floors – Existence of an elevator – Accessibility |
| Social profile | – Marital status – Number of children – Place of residence or care (selection menu) – Occupation – Last occupation – Care level – Care insurance benefits – Living will – Legal guardian – General power of attorney – Insurance number |
| Cost unit | – Exemption from co-payment – Name of the health insurance company (selection menu) – Responsible branch of the health insurance company – Postal address of the health insurance company – Date on which the insurance card was read. |
| Demographic data | – Age – Gender |
| Diagnoses and classifications | – Main diagnosis – Secondary diagnoses – Classifications – Onset of illness (MM-YYYY) |
| Clinical features and symptoms | – Symptoms – symptom onset (MM-YYYY) – symptom severity – progression variants |
| Measurement parameters, biomarker findings, genotype (if applicable) | – Body Mass Index (BMI) – Slow Vital Capacity (SVC) – Peak Cough Flow (PCF) – Neurofilament light chain (NF-L) in cerebrospinal fluid (CSF) – Neurofilament light chain (NF-L) in serum – Other biomarkers related to the principal diagnosis – Genotype related to the principal diagnosis |
| Respiratory care (if applicable) | – Non-invasive ventilation therapy (start: MM-YYYYY) – Invasive ventilation therapy (start: MM-YYYYY) |
| Nutritional care (if applicable) | – Non-invasive nutrition therapy (start: MM-YYYYY) – Invasive nutrition therapy (start: MM-YYYYY) |
| Provision of aids | – Completed medication (overview) – Current medication (overview) – Ticket number of the medication – Pharmacy central number (PZN) of the medication (if applicable) – Trade name of the medication – Ingredient of the medication – Dose of the medication — Date of start of medication (if applicable) — Date of end of medication (if applicable) — Dosage regimen—Dose of the medication – Start date of the medication – End date of the medication (if applicable) – Dosage regimen – Area of application (indication of the medication) – Supply partner (pharmacy) – Prescriber of the medication – Contact details of the prescriber |
| Medication | – Completed medication (overview) – Current medication (overview) – Ticket number of the medication – Pharmacy central number (PZN) of the medication (if applicable) – Trade name of the medication – Ingredient of the medication – Dose of the medication — Date of start of medication (if applicable) — Date of end of medication (if applicable) — Dosage regimen—Dose of the medication – Start date of the medication – End date of the medication (if applicable) – Dosage regimen – Area of application (indication of the medication) – Supply partner (pharmacy) – Prescriber of the medication – Contact details of the prescriber |
5. principle of multiple benefits
The AP concept is based on the basic principle of a multi-sided platform. In the platform structure, different partners make different contributions to the platform and generate role-specific benefits.
5.1. Benefits for patients
For patients and their relatives, the focus is on support in the search for suitable providers and relief in the organizational expenses involved in the long-term supply of medication. Patients and relatives who take part in care management benefit as follows, depending on the use of the APVP by the respective care partners:
- Support in the search for specialized and suitable suppliers
- Relief through contact persons for all supply issues
- Relief through organizational and administrative support in the provision, dispatch and storage of necessary statements, reports and other documents
- Relief through contact persons for complaints in care (complaints management of the coordinators)
- Strengthening autonomy through electronic medical records (EMR) including medication plan on the APVP (“empowerment”)
- Strengthening autonomy by displaying the status of assistive device supply (“Or is the assistive device in the approval process?”) on the APVP (“supply tracking”)
- Strengthening the active role of patients by inviting patient evaluations of medicines, aids and remedies, medical devices, medical services and providers
5.2. Benefits for medical partners
Medical partners who participate in APST’s care management benefit as follows:
- Quality gains through the option of transfer to specialized nonmedical care for complex, rare and chronic diseases (based on documented patient wishes)
- Strengthening own skills through patient feedback on care (patient evaluation)
- Strengthening your own skills by receiving statistics by e-mail on the initiated supply per month (initiated and delivered supply)
- Promotion of healthcare research projects (gaining knowledge; support for healthcare innovation)
5.3. Benefits for suppliers
For suppliers of medicines, there are considerable time and efficiency gains in data procurement. Furthermore, there are various advantages in quality management and the strengthening of differentiation features. The following benefits arise for suppliers who participate in supply management:
- Time and efficiency gains, as well as quality improvements in care through structured information on diagnoses, specific care goals and medical indications for care.
- Time and efficiency gains in the provision of care through the digital provision of patient and care-related data, including logistics data.
- Improving the quality of care by digitally providing patient and care-relevant data on special application conditions.
- Improving the quality of care by digitally providing patient and care-relevant data on special consultation circumstances.
- Time and efficiency gains as well as quality improvements through digital support for collaboration between the provider and other healthcare professionals.
- Quality control through structured patient evaluations (satisfaction survey on the provider’s services; benchmarking with other providers).
- Risk reduction of uneconomically incorrect care (through insight into existing and planned care for the same patient).
- Strengthening the provider profile and own specialization (through patient reviews and numerical display of previous care on the APVP).
- Participation in healthcare research projects (reputation gain; optimization of care processes).
5.4. Overall social benefit The overall perspective describes the benefits of care management that go beyond the perspective of a specific group of participants (patients, doctors, providers). The focus is on the support and relief of patients with serious and chronic illnesses through an innovative service architecture as well as the efficiency gain of care processes through digitalization. From an overarching perspective, digitally supported care management generates the following benefits:
- Relief for patients and their relatives with complex, rare and chronic diseases. Strengthening patient empowerment through patient assessments and coordinative services on behalf of the patient
- Strengthening specialization and differentiation processes in the provision of nonmedical services (neurologically specialized or sub-specialized therapy centers, medical supply stores and pharmacies)
- Efficiency gains for all stakeholders in complex care through a coordinating service and Internet platform (one-time collection of patient and care-related data, but multiple uses of the same data).
- Efficiency gains through digital change in supply processes (digital support for data and document management)
- Collection of “routine data” for the purpose of care optimization and care research (cross-payer and cross-provider data)
6. ensuring data protection and data security
The APVP internet platform is administered by APST, while patient-related data is stored in a protected database. APST ensures that data protection requirements are met. To this end, there is a cooperation between APST and Charité – Universitätsmedizin Berlin. Charité has taken over the hosting of the personal data. The data is stored in Charité’s data security architecture. In strict contrast to all forms of open Internet applications, the APVP is strictly confidential and only permitted for authorized users. Patients have expressly consented to the use of their data for the purpose of their outpatient care. The APST works exclusively with medical partners and care partners who have agreed to the use of patient data for the purpose of care research and strict compliance with data protection. The conditions of data protection are regulated in a separate data protection declaration. Consent to data protection by healthcare partners is a prerequisite for using the APVP internet platform.
7. provision and financing free of charge
The APVP’s services and software are provided free of charge for patients and their relatives, as charging fees is prohibited for psychosocial reasons. APST services for patients are financed from the fees charged by the care partners and from other forms of revenue (third-party funding of APST). APST services are also made available to medical partners free of charge, as these partners incur additional costs without any corresponding economic benefit. Patients and medical partners contribute to the financing of the APST concept by agreeing to the collection and use of healthcare research data (on the basis of informed consent), which is used scientifically and economically by APST (third-party funded APST projects). The use of care management services and the use of the APVP software is subject to a fee for care partners. Overall, the financing of the AP concept follows the “shared value concept”, in which the revenues of the APST (through fees from care partners and third-party funding) are used to create added value for society (free provision for patients).



